Medical Practice
Diagnose diseases with a sense of humanity
Examining the vasculature means evaluating individual patients. The field of vascular surgery is wide and requires abundant knowledge. When a patient with ischemic foot asked, “Why are my toes necrotic?”, we answered, “the arteries of your leg are obstructed with arteriosclerosis.” The patient also asked, “Why? What caused it?” We responded, “You have diabetes, hypertension, and have been smoking since you were young, right? And have you been exercising recently?”, to which the patient answered, “no.” Many factors are related to vascular diseases. Vascular surgeons imagine the life of patients in virtual synchronization from the moment they see them.
The operative indication depends on patients and their backgrounds. I will perform bypass surgery for lower limb ischemia in an 85-year-old man whose hobby is climbing mountains, but not for a 68-year-old woman with an ischemic foot after surgery for advanced gastric cancer with concomitant poor cardiac function. We discuss and carefully determine the timing of surgery; however, observation without surgery might be a good option in some cases. In vascular surgery, determining the operative indication automatically according to guidelines is sometimes not “appropriate.”
Fight against vascular diseases
In the words of Sun Tzu: “knowing, acquaintance, and a hundred battles.” In other words, “if you know the disease, the patient’s condition and the treatment methods you have, you will get better outcomes.” The first-line treatment method we have is surgery, which starts with a skin incision using a scalpel. However, endovascular treatments using catheters, wires, coils, stent grafts, etc., have emerged in succession and have dramatically improved minimally invasive surgery. In our department, there are skilled staff who have been trained in hospitals with a large number of cases, and we have demonstrated excellent outcomes. The Department of Vascular Surgery, University of Tokyo, has presented them at academic conferences and treaties.
Develop a strategy
The clinical conference (vascular board review) of vascular surgery is extremely exciting. The treatment decided at the conference may directly affect the patient’s fate. Although there are various guidelines, there are a wide variety of methods, including combinations of surgery and endovascular treatment, depending on the location of the lesion. The choice of strategy for one patient might differ between members of the conference and between facilities. Our motto is “evidence-based treatment” Doctors must explain properly, and all of them should be able to answer the question “Why is this strategy considered to fit your disease lesion?”.
Wide range of knowledge and skill
Vascular surgery is “surgery that deals with all vasculatures of the body except for the heart and brain”, and our staff has extensive knowledge about vascular diseases. Due to the nature of the university hospitals, we have been introduced to many rare diseases. There are many patients whose diseases were not diagnosed properly in other hospitals and finally came to our department where their disease was diagnosed and treated appropriately. In addition, we often encounter cases where surgery is very difficult or the nature of the disease is resistant to treatments (the bypass is quickly clogged or the anastomosis breaks down easily for unknown reasons); thus, we do our best as the last base and pursue good outcomes.
Vascular Team (medical collaboration)
It is not possible for a surgeon alone to treat all vascular diseases. Let me give you an example of a patient with severe lower limb ischemia and foot ulcers or necrosis. If there is an infection in the necrotic area, antibacterial treatment must be administered first, and an infectious diseases specialists should be consulted. Before bypass surgery in our department, we evaluate the peri- and intra-operative risks and routinely consult anesthesiologists and cardiologists. If, unfortunately, bypass is not possible, and a major amputation is required to prevent sepsis, we consult orthopedists. Collaboration with the rehabilitation department is necessary for future prosthesis preparation and patient-specific rehabilitation. Plastic surgeons can apply skin grafts and myocutaneous flaps on the skin defect lesion where the bypass has improved blood flow (plastic surgery). Diabetes and renal function have to be carefully monitored postoperatively by diabetologists and nephrologists, respectively, to improve the prognosis. Intractable ulcers often have vasculitis-related thrombosis, and the timing of surgery is decided in consultation with specialists in allergology and rheumatology.
We rely on the skill of laboratory technicians to evaluate blood vessels and their functions, both before and after surgery. The findings often change operative strategies. The cooperation of radiologists is sometimes important in difficult cases that require complicated endovascular procedures. In addition, foot care by a nurse (vascular nurse) can significantly change the outcome of ulcer healing.
In this way, vascular disease is treated through interdisciplinary collaboration. The vascular surgeon will act as a command tower.
Target diseases
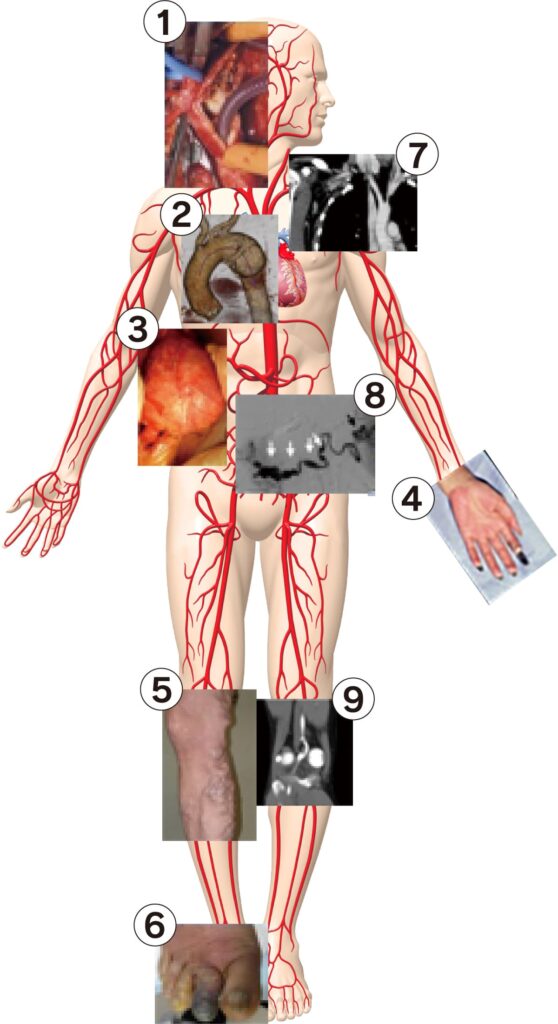
The target diseases of vascular surgery vary widely as shown in the figure.
Frequent vascular diseases
- Carotid artery stenosis①
- Thoracic aortic aneurysm②
- Abdominal aortic aneurysm③
- Aortic dissection
- Vascular trauma
- Buerger disease④
- Acute arterial occlusion
- Leg varix⑤
- Deep vein thrombosis
- Lymphoedema
- Arteriosclerosis obliterans of lower extremity⑥
Rare vascular diseases
- Thoracic outlet syndrome⑦
- Takayasu’s disease (aortitis syndrome)
- IgG-related diseases
- Visceral aneurysms and SAM⑧
- Peripheral artery aneurysm
- Vascular Behçet’s disease
- Popliteal artery entrapment syndrome⑨
- Adventitial cyst of the popliteal artery
- Congenital arteriovenous malformation
- Raynaud’s disease
- Residual ischial artery
etc.
Main vascular diseases and operative strategies/policies
We describe some of the vascular diseases treated in vascular surgery and the treatment strategies from our unique perspective.
There are many other diseases besides the ones below, and we plan to upload them soon.
- Treatment for the abdominal aortic aneurysm
- Treatment for the arteriosclerosis obliterans
- Treatment for cervical artery stenosis
- Stent graft for the thoracic aortic aneurysm
- Treatment for the leg varix
- Visceral artery aneurysm
- Treatment strategy for the splenic artery aneurysm
- What centimeter in diameter of the iliac artery aneurysm should be the high risk of rupture?
- What is Ehlers-Danlos syndrome?